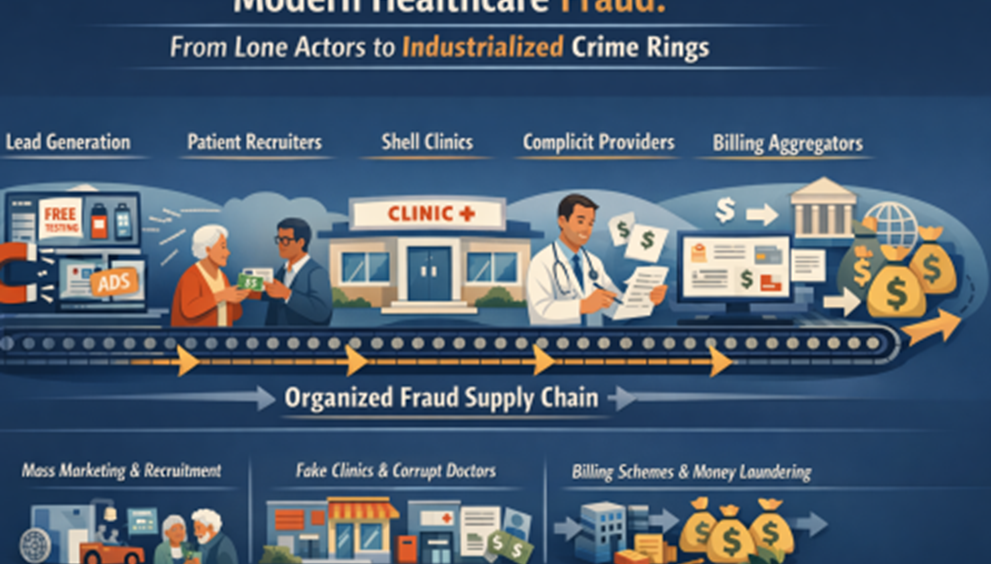
‘The Fraud Supply Chain’: How Healthcare Fraud Is Industrialized
Healthcare fraud has evolved beyond the image of lone individuals falsifying claims or inventing phantom treatments into full-on fraud factories with supply chains. Today’s schemes resemble sophisticated, multi-faceted organized businesses: specialized teams handle lead generation, patient recruitment, shell clinics, complicit providers, billing aggregation, and money laundering.
In 2025 alone, a coordinated National Health Care Fraud Takedown taskforce charged 324 defendants in connection with more than $14.6 billion in alleged fraudulent activity — the largest such action in U.S. history — including 96 licensed clinicians across 50 federal districts and 12 state attorney general offices. Those schemes exploited vulnerable patients and taxpayers and involved transnational elements and complex networks of shell entities.
Lead Generation
To outpace rivals and grow revenue, fraudsters manufacture beneficiary demand. They run targeted marketing — often through compelling ads for pain relief, “free” medical equipment, or genetic testing — then scrape public directories for provider data (names, addresses, national provider IDs and taxonomy codes) and harvest beneficiary info from other publicly accessible sources.
In one high-profile genetic testing fraud case, telemarketing operators in Texas and Florida recruited Medicare beneficiaries for medically unnecessary cancer genetic (CGx) testing that was not eligible for reimbursement, resulting in more than $17 million in billed claims, with over $5.2 million paid out.
High-volume call centers then pitch these “free” services to vulnerable seniors via mass dialing, social campaigns, and other outbound methods.
Patient Recruiters
Contacted beneficiaries are recruited with cash, gift cards, or free transportation. Recruiters often target seniors, Medicaid recipients, individuals in recovery, and residents of rural communities — sometimes at churches, senior centers, and community events — to maximize attendance in group sign-ups.
Once patients agree, the recruiter hands them off to a clinician or telehealth provider who signs an order, completing the fraud “supply chain” that enables billing. Recent enforcement actions have shown how aggressive phone-based solicitation and inducements can be central to scheme initiation.
Shell Clinics
Networks form shell companies with fake websites, rented credentials, or stolen national provider IDs (NPIs) to create the infrastructure necessary for billing. The low overhead and rapid scalability of telehealth — combined with minimal in-person clinical oversight — have made such models especially attractive.
In the 2025 takedown, prosecutors alleged that some schemes used foreign straw owners and nominee companies to enroll dozens of durable medical equipment and laboratory businesses that submitted fraudulent claims exceeding $10 billion in false Medicare billings.
Complicit Providers
Legitimate providers can be linchpins in industrialized fraud rings by knowingly participating for extra income in the form of flat fees, volume-based kickbacks, or credential rentals. These arrangements, which constitute conspiracy to falsify claims, are a frequent target of enforcement.
For example, in one genetic testing fraud scheme, call center operators not only recruited beneficiaries but also falsified laboratory ownership documents to enroll a clinical lab in Medicare, leading to sentencing and orders for millions in forfeiture and restitution.
Billing Aggregators
Aggregators compile signed orders into clean, reimbursable claims; optimize coding for maximum rates; monitor denials; and standardize documentation for repeatability. They focus on high-value areas like durable medical equipment, behavioral health, and laboratory testing — acting as revenue engineers.
The scale of these operations was confirmed in the 2025 takedown, when civil settlements, provider sanctions, and asset seizures exceeded $245 million alongside the criminal charges — underscoring the coordinated role billing and administrative networks play in scaling schemes.
Money Laundering
Once funds are paid, they are drained quickly from receiving accounts, routed through multi-state shell companies, fragmented into smaller transactions, and disguised as consulting, marketing, or management fees. Speed and layering distance proceeds from their origin while complicating enforcement.
In the same 2025 takedown, authorities reported that some defendants allegedly conspired to conceal and launder fraud proceeds, including international transfers and high-value asset purchases like a $2.9 million home in Dubai, highlighting how proceeds are moved far beyond where the scheme originated and the supply chain began.
A Practitioner’s Closing Thought
Today’s fraud rings thrive on industrialization: compartmentalized roles limit visibility and boost efficiency, burdening investigators while enabling scale. Fraud fighters must shift from viewing cases as isolated to treating them as connected businesses. Early supply chain signals — suspicious ads, beneficiary calls, shared marketing assets — deserve scrutiny, and analysts should trace spikes back to campaigns. Shared leads across unrelated providers, common billing services among suspicious clusters, and identical marketing messages driving geographically dispersed claims expose networks. Graph analytics and network analysis are essential tools in combating industrialized fraud effectively.
Healthcare fraud has become a factory — and prevention and investigation must combat it as one.